Most people booking a hair transplant rarely ask the most useful question first. They want to know how many grafts they need, what the price will be, how long the trip takes. All valid. But the number that quietly decides the long-term result is something else entirely: how many of those grafts actually survive once they’re in place. With percutaneous hair transplantation, that number tends to be encouraging — though it’s never a flat guarantee.
Table of Contents
What Percutaneous Hair Transplantation Actually Means
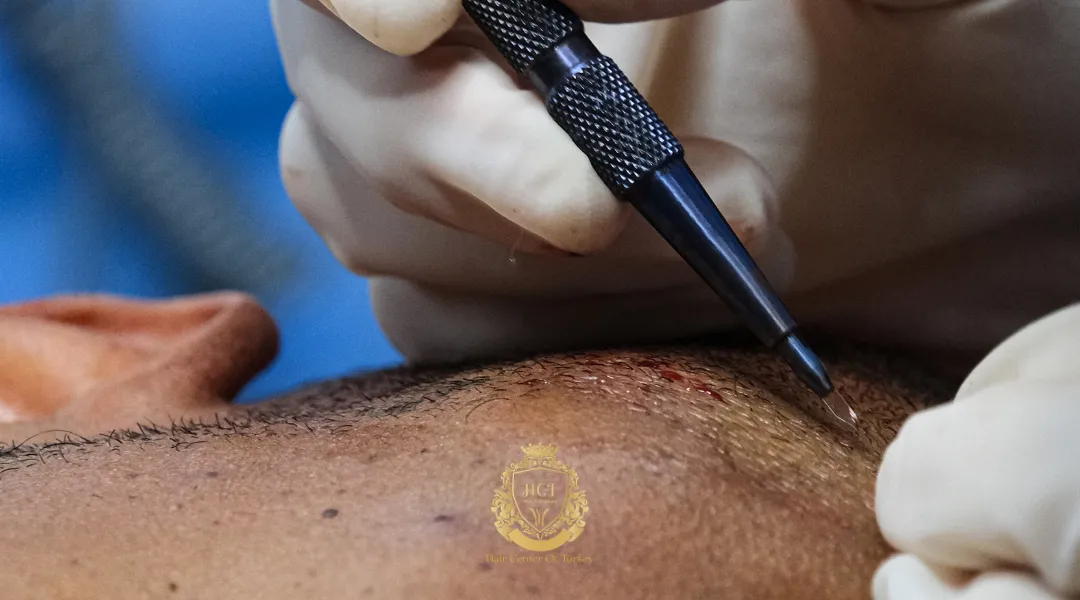
Percutaneous transplantation, often called the implanter pen method or pen-based DHI, places each follicular unit directly into the scalp through a fine, hollow tip. There’s no separate channel-opening step in the traditional sense. The tip creates the opening and delivers the graft in one motion. Less handling. Less drying. Less time outside the body. That alone changes the math on survival.
The Real Numbers: How High Can Graft Survival Go?
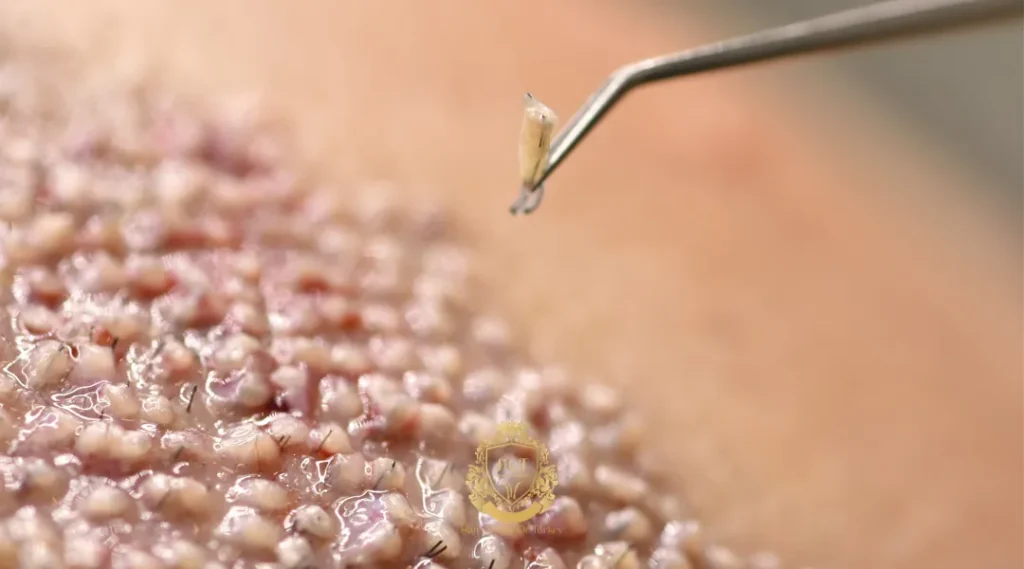
In well-run clinics, percutaneous procedures typically report a graft survival rate somewhere around 90 to 95 percent. Some experienced teams claim higher, and in straightforward cases that’s plausible. But honest framing matters here. A single fixed number is misleading on its own. Survival depends on biology, technique, timing, and how the patient behaves after the procedure. Anyone promising a guaranteed 100% should be approached with a healthy dose of caution.
What Drives the Survival Rate Higher (or Lower)
Several factors shape how many grafts actually take. Some are clinical, some are practical, and a few are simply about discipline.
- Time grafts spend outside the scalp before placement
- Holding solution quality and temperature control
- Density of placement — too tight reduces blood supply
- Angle and depth of insertion
- Patient’s general health, smoking status, and scalp condition
- How carefully the first 10 to 14 days are managed at home
Pull any one of these out of balance and the curve drops. It’s rarely a single dramatic mistake. Usually it’s small, accumulated friction across a long day.
Why the Implanter Pen Tends to Protect Grafts
The pen design has a clear purpose. It shields the follicle inside its hollow channel from the moment it’s loaded until the moment it lands in the scalp. That short journey matters. Open exposure to air, repeated forceps contact, and channel-graft mismatch are common sources of trauma in older techniques. With a well-handled pen, grafts move from holding solution to scalp in seconds, in one motion. Less drama for the follicle, generally better odds for it.
Surgeon Skill, Team Coordination, and the Quiet Variables
People underestimate how much team rhythm shapes the outcome. A percutaneous case usually runs with a lead surgeon and a small group of trained technicians working in sync. If extraction lags, grafts wait. If implantation rushes, depth gets sloppy. The survival rate is, in a real sense, a measure of how calm and consistent that choreography is across six or seven hours. So the clinic you pick isn’t just a brand — it’s a working group with habits.
Aftercare Matters More Than People Realise
The procedure ends, but the grafts aren’t anchored yet. The first two weeks are when most of the survival math is finalised. A graft that took beautifully on the table can still be lost to a careless night, a tight cap, or an aggressive shower head.
Practical post-op behaviours that quietly protect your result:
- Sleep on your back with the recommended neck pillow for the first nights
- Avoid sweating, gym sessions, and sauna for at least 10 to 14 days
- Follow the spray and washing schedule precisely — not loosely
- Stay off alcohol and nicotine in the early window
- Don’t pick at scabs, even when they itch
None of this is glamorous. But it’s where good surgeries are quietly saved, or quietly damaged.
How Hair Center of Turkey Approaches the Process

In structured clinics such as Hair Center of Turkey, a percutaneous procedure usually starts long before the chair. The donor area is mapped, the hairline is drawn with the patient’s facial structure in mind, and the graft count is calibrated to what the donor can actually spare without thinning out. Method selection follows the patient, not the trend. That ordering matters. When planning is done properly, the procedure itself becomes the easier half. Communication then continues after travel home — which, for international patients, tends to be the part most clinics under-deliver on.
Comparing Percutaneous to FUE and DHI in Survival Terms
In capable hands, all three modern techniques can deliver high graft survival. The honest comparison is about workflow, not magic. Classic FUE separates channel opening from implantation, which gives flexibility but adds graft handling time. DHI uses a Choi-style implanter and shortens that gap. Percutaneous, in its refined pen-based form, sits in the same family as DHI and chases the same goal: less handling, faster placement, denser yet safe distribution. So the more useful question isn’t which technique has the best survival rate. It’s which technique fits this patient — and which team will actually execute it well.
Final Thoughts
Graft survival in percutaneous transplantation is high, but it’s earned, not handed out. The technique offers real biological advantages: short transit time, controlled placement, less trauma to the follicle. What turns those advantages into a visible result is the layer around the technique — planning, team coordination, donor management, and the patient’s own care in the weeks that follow. A clinic that takes that whole arc seriously, like Hair Center of Turkey, gives the procedure a quieter, more predictable shape. And usually, that’s what separates a good outcome from a frustrating one.
FAQ
What graft survival rate is realistic with percutaneous hair transplantation?
Most experienced clinics report a survival rate in the 90 to 95 percent range. Higher figures are possible in clean, well-managed cases, but a guaranteed 100 percent is not a medically honest claim and should be treated with skepticism.
Does percutaneous give better results than classic FUE?
It depends on the patient. Percutaneous shortens graft transit time and supports denser placement, which often helps survival. But a skilled FUE team can match it. Technique matters less than the team executing it.
How soon can I tell if my grafts are surviving well?
Real visibility usually appears between months four and eight. Earlier shedding around weeks two to six is normal and not a sign of failure. Patience in this window is part of the process.
What hurts graft survival the most after the procedure?
Sweating, smoking, alcohol, scab picking, and ignoring the washing routine. Mechanical pressure on the recipient area during the first two weeks is also a common, avoidable cause of loss.
Is percutaneous a sensible choice for a first-time international patient?
Often yes, especially when the clinic plans the case before travel and supports aftercare remotely. With a clear graft plan and proper communication, the journey becomes considerably more manageable from abroad.




